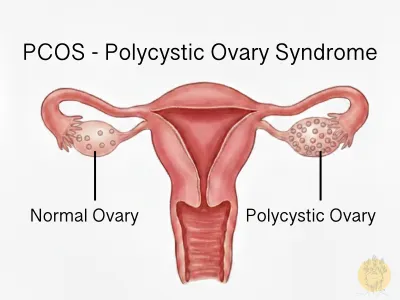
What is PCOS?
Polycystic ovary syndrome (PCOS) is a hormonal disorder that happens when your ovaries produce too much androgen, a group of hormones that are typically present in small amounts in women. This hormonal imbalance disrupts your reproductive cycle, which is why women with PCOS often experience irregular periods, missed periods and unpredictable ovulation. When ovulation does not happen regularly, small fluid-filled follicles can build up on the ovaries, and that is where the “polycystic” in the name comes from. That said, you do not need to have these follicles visible on an ultrasound to be diagnosed with PCOS.
PCOS is one of the leading causes of female infertility in the United States and affects an estimated 5 million American women. But it goes beyond reproductive health. Because insulin resistance is often at the root of it, PCOS also raises your risk for type 2 diabetes, cardiovascular disease, and metabolic dysfunction. The good news is that with the right approach targeting the actual cause rather than just the symptoms, most women see significant improvement.
What Causes PCOS?
PCOS develops from a combination of hormonal imbalances, metabolic dysfunction and genetic predisposition that feed into each other in a cycle that can be difficult to break without the right intervention.

Androgen Excess and Hyperandrogenism
The primary driver behind PCOS is an overproduction of androgens. Androgens are hormones like testosterone and DHEA that play a role in male development but are also produced in smaller amounts by every woman. When androgen levels become elevated, a state called hyperandrogenism, the ovaries are prevented from releasing an egg each month. This disruption in ovulation is what leads to irregular periods, missed cycles and many of the visible symptoms like acne, excess hair growth and thinning hair on the scalp.
More than 80% of women who present with signs of hyperandrogenism are eventually diagnosed with PCOS. The excess androgens can come from the ovaries, the adrenal glands or both, and the source often determines the specific pattern of symptoms a woman experiences.
Insulin Resistance and Hyperinsulinemia
When your body becomes resistant to insulin, your cells stop responding to it efficiently. The pancreas compensates by producing more and more insulin, a state known as hyperinsulinemia, and that excess insulin directly signals the ovaries to produce more androgens.
Higher insulin leads to higher androgens, which worsens PCOS symptoms, which can lead to weight gain, which further increases insulin resistance. This is also why conditions like hypothyroidism need to be ruled out during diagnosis, since they can share overlapping metabolic features with PCOS.
Gonadotropin Imbalance: LH and FSH
Women with PCOS often have an imbalance in the two hormones that regulate ovulation, luteinizing hormone (LH) and follicle stimulating hormone (FSH). In a normal cycle, LH and FSH work in a coordinated rhythm to mature a follicle and trigger the release of an egg. In PCOS, LH levels tend to be elevated while FSH stays relatively low.
This altered LH to FSH ratio disrupts the normal ovulation process. The follicles begin to develop but never fully mature. Instead of releasing a healthy egg, the ovary accumulates small immature follicles, which is what creates that polycystic appearance on an ultrasound.
PCOS Symptoms
Menstrual and Reproductive Symptoms
Irregular, infrequent or completely absent periods caused by oligo-anovulation
- Cycles longer than 35 days or fewer than nine periods per year
- Unusually heavy bleeding when a period does occur
- Difficulty getting pregnant due to lack of ovulation, making PCOS one of the leading causes of female infertility
Skin and Hair Changes
- Persistent hormonal acne along the jawline, chin, chest and upper back that does not respond to standard treatments, driven by excess androgens like testosterone and DHT
- Thinning hair on the scalp (androgenic alopecia) particularly at the crown and part line, caused by the 5 alpha reductase enzyme converting testosterone to DHT
- Excess thick dark hair growth on the face, chest, abdomen and inner thighs known as hirsutism, affecting up to 70% of women with PCOS
- Dark skin patches called acanthosis nigricans on the neck, underarms and groin, a visible marker of insulin resistance rather than a skin condition on its own
- Skin tags commonly found on the neck and underarms
Metabolic and Systemic Symptoms
- Weight gain concentrated around the midsection commonly referred to as PCOS belly, driven by insulin resistance and excess insulin promoting visceral fat storage
- Increased risk of type 2 diabetes, elevated lipids, cardiovascular disease and nonalcoholic steatohepatitis
- Obstructive sleep apnea affecting approximately 35% of women with PCOS, even those who are not overweight
- Depression and anxiety at rates roughly four to six times higher than women without PCOS, linked to both androgen driven neurotransmitter disruption and the emotional toll of living with visible hormonal imbalances
How is PCOS Diagnosed
PCOS is a diagnosis of exclusion, meaning other conditions must be ruled out before it is confirmed. Most providers use the Rotterdam Criteria which require at least two of the following three findings:
- Clinical or biochemical hyperandrogenism (elevated testosterone, DHEA-S or visible signs like acne, hirsutism and thinning hair)
- Oligo-anovulation (irregular, infrequent or absent periods)
- Polycystic ovarian morphology on ultrasound (20 or more follicles per ovary measuring 2 to 9 mm or ovarian volume greater than 10 mL)
Common Lab Tests and Imaging
- Total and free testosterone to assess androgen excess
- DHEA-S to evaluate adrenal androgen production
- LH and FSH ratio to check for gonadotropin imbalance
- Fasting insulin and glucose to screen for insulin resistance
- HbA1c or 2 hour oral glucose tolerance test to assess diabetes risk
- Fasting lipid panel for cardiovascular risk
- AMH (anti-Mullerian hormone) as an alternative marker for polycystic ovarian morphology
- Pelvic ultrasound to visualize the ovaries and count follicles
- Progesterone levels to confirm whether ovulation is occurring
Conditions That Must Be Ruled Out
- Hypothyroidism (via TSH)
- Hyperprolactinemia
- Nonclassical congenital adrenal hyperplasia (via 17-hydroxyprogesterone)
- Cushing syndrome (via cortisol testing)
- Hypogonadotropic hypogonadism
- Androgen secreting tumors (suspected when levels are extremely elevated or symptoms develop rapidly)
If you are currently on hormonal birth control, lab results for hyperandrogenism may not be accurate. Most providers recommend stopping hormonal contraceptives for at least three months before testing to get a reliable picture of your hormone levels.
PCOS Treatment and Medication
There is no single cure for PCOS, but the right combination of treatments can significantly reduce symptoms and lower the risk of long term complications. PCOS treatment is individualized based on the severity of symptoms, metabolic markers and whether or not pregnancy is a goal.
Conventional Treatments
Birth Control and Hormonal Contraceptives
Combined oral contraceptive pills are the first line PCOS medication for managing irregular periods, acne and hirsutism in women who are not trying to conceive. Birth control works by suppressing androgen production, increasing sex hormone binding globulin (SHBG) and regulating the menstrual cycle. However, it is important to understand that birth control does not address the underlying insulin resistance or hyperandrogenism driving the condition. It manages symptoms while you are on it but does not resolve the root cause.
Metformin for Insulin Resistance
Metformin is an insulin sensitizing drug originally developed for type 2 diabetes that has become a cornerstone in PCOS treatment. It helps the body use insulin more effectively, lowers circulating androgen levels, improves menstrual regularity and supports weight loss. Current guidelines recommend metformin for PCOS primarily in women with a BMI of 25 or higher to manage metabolic features like insulin resistance and abnormal lipid levels.
Spironolactone and Anti-Androgens
Spironolactone is an androgen receptor blocker commonly prescribed for hirsutism, hormonal acne and thinning hair in women with PCOS. It typically takes at least six months to show visible improvement in hair growth and is often combined with birth control since it is not safe during pregnancy. Research shows that combining spironolactone with metformin can be more effective for reducing insulin resistance and testosterone levels than either drug alone.
Fertility Medications
For women trying to get pregnant, letrozole is now the preferred first line fertility medication for PCOS related anovulatory infertility. Studies show it produces higher ovulation and birth rates compared to clomiphene citrate. Clomiphene combined with metformin is another commonly used option. In more resistant cases, gonadotropin injections or IVF may be considered.
Functional Medicine Approach
A functional medicine approach to PCOS focuses on identifying and addressing the metabolic root of the condition rather than only managing symptoms with medication.
Targeted Supplements
- Myo-inositol improves insulin sensitivity, supports ovulation and has been shown to be comparable to metformin with fewer side effects
- Berberine functions as a natural insulin sensitizer and has been studied as an alternative to metformin for lowering blood glucose and androgen levels
- Alpha lipoic acid improves insulin sensitivity and supports healthy glucose metabolism
- Chromium helps regulate blood sugar and reduce insulin resistance
- NAC (N-acetylcysteine) has been shown to improve ovulation rates and lower testosterone
- Gymnema supports blood sugar regulation and healthy insulin response
Herbal Support for Androgens
- Licorice root and peony to help lower excess androgens
- Spearmint tea and chamomile to reduce testosterone levels naturally
- Saw palmetto, nettle root, pygeum, EGCG and reishi mushroom to inhibit the 5 alpha reductase enzyme that converts testosterone to DHT
- Adaptogens and stress management techniques to modulate cortisol and support hormonal balance
PCOS Diet: What to Eat and What to Avoid
Foods That Support Insulin Sensitivity
- Leafy greens like spinach, kale and broccoli for fiber and anti-inflammatory nutrients
- Berries, apples and citrus fruits that are lower in sugar and high in antioxidants
- Wild caught salmon, sardines and mackerel rich in omega 3 fatty acids that reduce inflammation and improve insulin sensitivity
- Avocados, olive oil, nuts and seeds for healthy fats that support hormone production
- Legumes, lentils and beans for plant based protein and slow releasing carbohydrates
- Whole grains like quinoa, oats and brown rice that prevent blood sugar spikes
- Lean proteins including chicken, turkey, eggs and tofu to promote satiety without triggering excess insulin release
Foods to Limit or Avoid
- Refined carbohydrates like white bread, white rice and pastries
- Sugary beverages including soda, juice and sweetened coffee drinks
- Processed and fried foods high in trans fats and saturated fats
- Red and processed meats like hot dogs, bacon and fast food burgers
- Added sugars hidden in cereals, yogurts, sauces and packaged snacks
- Excess dairy which may trigger higher postprandial insulin release in some women with PCOS
PCOS and Weight Loss
PCOS weight loss is challenging because insulin resistance promotes fat storage, particularly around the abdomen. But even a 5% reduction in body weight has been shown to improve ovulation, regulate menstrual cycles, lower testosterone and improve insulin sensitivity. The key is pairing a low glycemic, anti-inflammatory diet with consistent physical activity and metabolic support rather than relying on extreme calorie restriction which can backfire hormonally. Eating smaller balanced meals every three to four hours helps maintain steady blood sugar and prevents the insulin spikes that drive PCOS symptoms.
Best Exercises for PCOS
Resistance training is particularly effective for women with PCOS because it builds lean muscle mass, which acts as a metabolic sink for glucose.
Recommended Movements and Frequency
- Squats, lunges and leg presses targeting the quadriceps, hamstrings and glutes
- Deadlifts and hip thrusts for posterior chain activation
- Push ups, bench presses and shoulder presses for upper body strength
- Rows and pull downs to engage the back and core
Other Beneficial Activities
- Walking for 30 minutes daily as a baseline for blood sugar management
- High intensity interval training (HIIT) which has been shown to improve insulin resistance, lower LDL cholesterol and reduce testosterone levels in women with PCOS
- Yoga and mindfulness based movement for cortisol regulation and stress reduction, both of which impact androgen production and hormonal balance
- Swimming and cycling as low impact options that still support cardiovascular health and PCOS weight loss
PCOS and Pregnancy
Why Fertility is Affected
PCOS disrupts female fertility because of oligo-anovulation. When androgen levels are elevated and insulin resistance is present, the normal balance of LH and FSH is thrown off. Without that hormonal coordination, the ovaries cannot mature and release an egg each cycle. No ovulation means no egg available for fertilization. Progesterone levels also drop because progesterone is only produced after ovulation occurs, and estrogen can fluctuate unpredictably.
How to Restore Ovulation Naturally
- Reducing insulin resistance through a low glycemic diet, resistance training and targeted supplements like myo-inositol and berberine
- Lowering androgen levels with herbal support such as spearmint, licorice root and peony
- Achieving even a modest 5% weight loss which has been shown to restore ovulatory cycles in many women
- Working with a provider to evaluate whether medications like letrozole, clomiphene or metformin are appropriate for your specific situation
Letrozole is currently the preferred first line fertility medication for PCOS related anovulatory infertility, with studies showing higher ovulation and live birth rates compared to clomiphene alone. Clomiphene combined with metformin is another effective option. In more complex cases, gonadotropin injections or IVF may be recommended.
Frequently Asked Questions on PCOS
Can you get pregnant with PCOS?
Yes. PCOS is a leading cause of female infertility but it does not mean you cannot conceive. The main barrier is absent ovulation caused by excess androgens and insulin resistance. Once ovulation is restored through lifestyle changes or medications like letrozole and metformin, many women with PCOS have healthy pregnancies.
What causes PCOS?
The primary driver is overproduction of androgens like testosterone and DHEA. Insulin resistance fuels this by signaling the ovaries to produce more male hormones. Genetics, chronic inflammation, obesity and gonadotropin imbalance all contribute to the development of polycystic ovary syndrome.
What does PCOS pain feel like?
Some women with PCOS experience a dull aching pressure in the lower abdomen related to enlarged ovaries with multiple follicles or heavy prolonged bleeding. Not everyone with PCOS experiences pain, but when present it is often described as persistent heaviness rather than sharp cramping.
How can you tell if you have PCOS?
The most reliable way to confirm a PCOS diagnosis is through your healthcare provider using the Rotterdam Criteria, which evaluates hyperandrogenism, oligo-anovulation and polycystic ovarian morphology on ultrasound. If you are experiencing irregular periods, stubborn acne, unexplained weight gain or excess hair growth, these are signals worth getting evaluated through blood work and imaging.
What are the worst symptoms of PCOS?
The most distressing PCOS symptoms reported by women include infertility, stubborn PCOS belly weight gain, severe hormonal acne, excessive facial hair and thinning hair. The metabolic complications like insulin resistance, elevated cardiovascular risk and increased chance of type 2 diabetes are often the most dangerous long term even when they are less visible.
What is the best way to control PCOS?
The most effective approach combines a low glycemic anti-inflammatory diet, regular exercise with emphasis on resistance training and targeted support like myo-inositol, berberine or metformin to address insulin resistance. Birth control and spironolactone manage surface symptoms like acne and hirsutism but addressing the metabolic root through lifestyle changes produces the most sustainable results. Watch the attached youtube shorts on this page to better understand the steps to take.
What is the best thing to do for PCOS?
Start with the foundations. A PCOS diet built around whole foods, lean proteins, healthy fats and low glycemic carbohydrates paired with strength training at least three times per week can meaningfully improve insulin levels, androgen production and ovulation. Working with a provider who understands the metabolic side of PCOS rather than just prescribing birth control makes a significant difference in long term outcomes.
What does PCOS do to a woman?
PCOS affects far more than just the reproductive system. Elevated androgens and insulin resistance disrupt ovulation, trigger acne, hirsutism, thinning hair and abdominal weight gain while increasing long term risk for type 2 diabetes, cardiovascular disease, sleep apnea and mood disorders. It is both an endocrine and metabolic condition that requires comprehensive management beyond just symptom suppression.